Do you know how patients really feel when visiting your oncology office? We recently partnered with OnePoll to survey 2,005 Americans about their opinions on in-office visits across multiple specialties. Here are three ways we found that you can be improving the patient experience at your practice.
More Patient Education
When asked what they wished their healthcare provider would do during appointments, 59% of respondents wanted their provider to give more educational materials on their condition/symptoms. And 55% wanted their provider to speak in more detail about their treatment/medication.
Patients want to fully understand their diagnosis, but they’re concerned that you won’t be able to explain it in a way that makes sense for them. 69% of respondents feared their HCP would use terminology that they wouldn’t understand. This highlights the importance of using plain language when describing diagnoses and treatment plans.
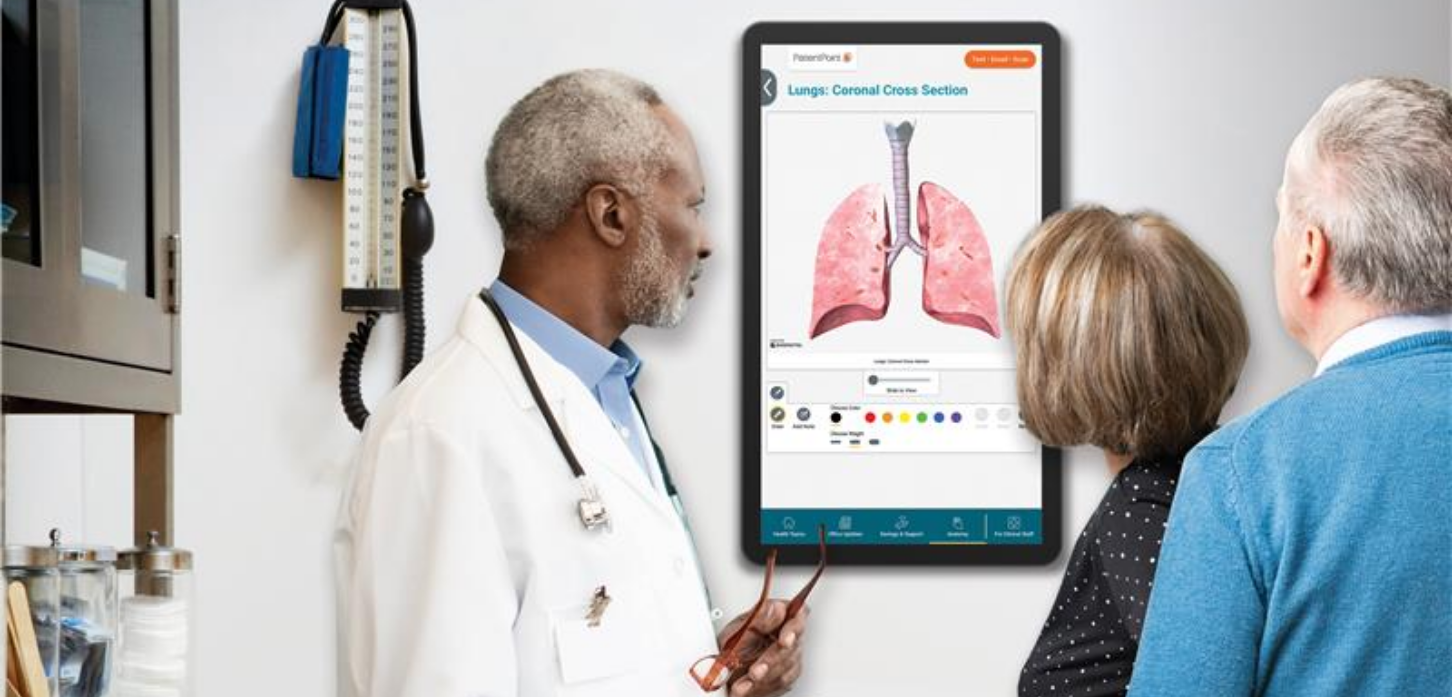
The right technology can also help you explain their cancer. And consider that 78% wanted the doctor’s office to feel more modern by adding technology showcasing relevant education on their condition/symptoms.
Better Waiting Experiences

Patients spend a significant amount of time waiting in the office, and this only exacerbates any anxiety they were already experiencing beforehand. At the end of 2022, we found that oncology patients were waiting 14.2 minutes in the waiting room and 11.4 minutes in the exam room on average.1
51% of patients believed it takes too long to be called for their appointment, and 48% said it takes too long to be seen by their healthcare provider once they’re in the exam room. You can make the wait less stressful and more educational by adding a digital platform. We recommend having screens in both the waiting room and exam room that share wellness messages, treatment guides, tips on managing side effects and more cancer-specific content to boost health literacy.
This will also help patients prepare for discussions with their doctor and may make the visit a more positive one. 69% of patients felt negatively toward their doctor’s visit because they wished they knew how to describe their condition/symptoms better before talking to their healthcare provider.
Learn more about oncology wait times in 2022 in our blog.
Improved Health Equity
Another insight we gathered was that different demographics experience different amounts of stress in the office. 65% of Black Americans said it was very or somewhat difficult to find a doctor who shares the same background and experience as them, compared to 54% of Hispanic Americans and 40% of White Americans.2
Unsurprising then, White respondents trusted doctors the most to do what was right for them or their community almost all or most of the time. These statistics point to an opportunity for you to increase health equity in your practice. This is a major goal of the upcoming Enhancing Oncology Model (EOM) as well.
If you will be an EOM participant, you will need to be performing redesign activities, including screening for health-related social needs and providing 24/7 access to care. Even if you’re not joining the model, it may be worth adding some of these redesign activities to better meet the needs of every patient.
Check out all of the insights we discovered in our survey by reading our e-book. And learn more about EOM straight from an oncologist in our interview with Dr. Kashyap Patel.
1“During your most recent visit to your healthcare professional about how many minutes did you spend…?” 2021-2022 Nationwide Web Surveys of 11,198 respondents who visited physician offices installed with the PatientPoint Communicate, Educate, and/or Interact Programs. Data as of 12/31/22
2Hamel L, Lopes L, Muñana C, Artiga S, Brodie M. KFF/The Undefeated Survey on Race and Health. October 13, 2020. https://www.kff.org/racial-equity-and-health-policy/report/kff-the-undefeated-survey-on-race-and-health/
3Unless otherwise stated, all information was received from a OnePoll study conducted on PatientPoint’s behalf from Sept. 22nd to Sept. 30th, 2022 with 2,005 nationally representative Americans.

